Chelsea Heights Chiropractic
Get back to
the life
you love.
Evidence-informed chiropractic care and Stecco Fascial Manipulation — addressing root causes, not just the site of pain.
Serving Chelsea Heights and Melbourne's Bayside south-east.
Over 23 years in practice.
23+
Years in
practice
practice
60min
Allow for your
first visit
first visit
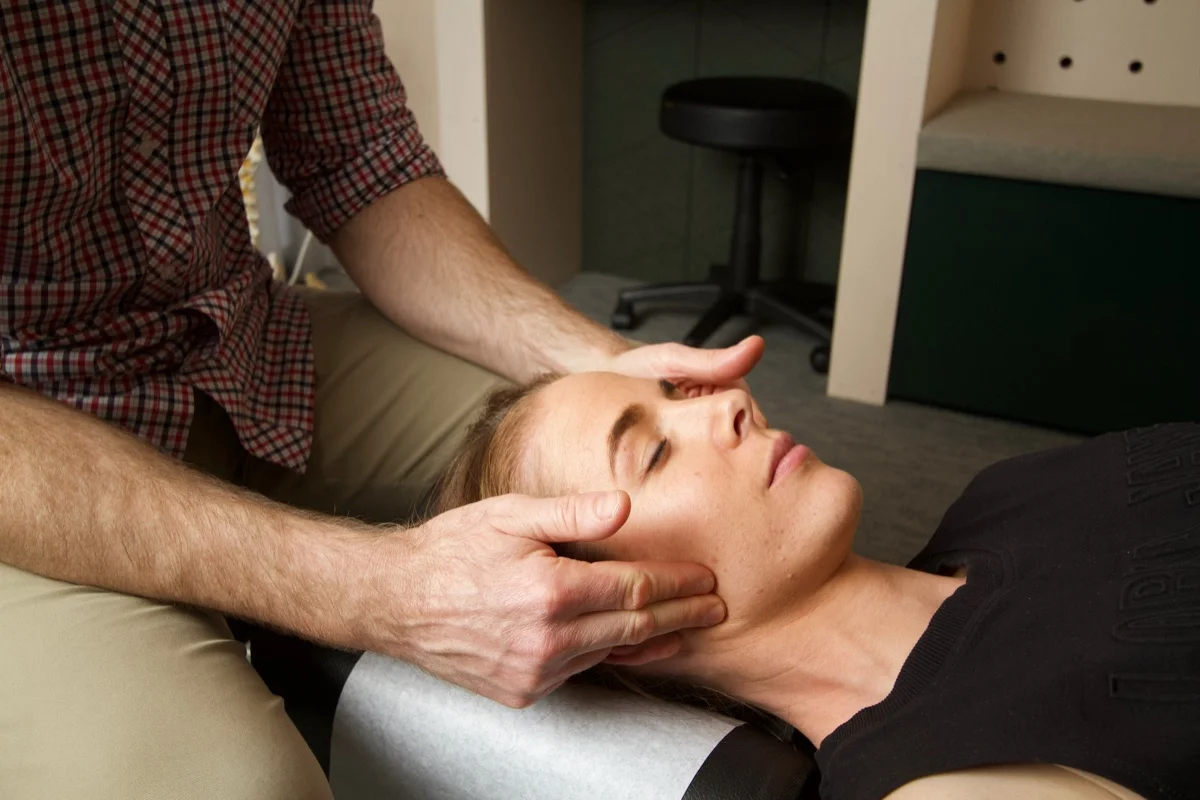
New patients — what to expect
Full movement & fascial assessment
Working diagnosis — explained clearly
Treatment begins at visit one
Our approach
Your body is an
interconnected
masterpiece.
Focusing on a single painful area in isolation rarely yields lasting results. Pain location is frequently misleading — the root cause is often found elsewhere in the body entirely.
We assess overall movement patterns alongside localised findings to make rational decisions about your management — and get you back to what you love, faster.
Our philosophy01
A precisely targeted manual therapy addressing densified fascia — the connective tissue that links your entire body. Where other treatments address symptoms, this targets the root cause.
02
Specific spinal and extremity manipulation to restore joint mobility, reduce pain, and optimise neural function. Twenty years of clinical experience informing every decision.
03
Cervicogenic headache, tension-type headache, migraine management, BPPV, and cervicogenic dizziness. An area of deep clinical interest — and one where fascial and neurological assessment makes a significant difference.
New to the clinic?
What to expect
as a new patient.
1
Book Online
Choose a time that suits. Allow 60 minutes for your first appointment.
2
Full Assessment
Thorough history and examination — not just the painful area. We look for the pattern behind the problem.
3
Clear Diagnosis
You'll leave understanding what's happening, why, and what the plan looks like. No jargon, no vagueness.
4
Get Moving
Treatment begins at your first visit. Most patients notice meaningful change within 2–3 appointments.
Evidence-informed care
Conditions we treat.
Lower Back & Pelvis
Disc injuries, lumbar facet syndrome, SIJ dysfunction, piriformis syndrome, myofascial pain, and cluneal neuralgia — viewed through the fascial system that connects them all.
Learn more
Neck, Headache & Dizziness
Cervicogenic headache, tension-type headache, migraine, cervical radiculopathy, BPPV, and cervicogenic dizziness. The cervical spine is at the centre of more conditions than most people realise.
Learn more
Shoulder
Rotator cuff tendinopathy, subacromial bursitis, shoulder impingement, and biceps tendinopathy. Shoulder pain rarely begins at the shoulder — thoracic mobility and scapular control are assessed every time.
Learn more
Knee
Patellofemoral pain, ITB syndrome, and patellar tendinopathy. Knee pain is rarely just a knee problem — hip mechanics and foot posture are assessed every time.
Learn more
Hip
Gluteal tendinopathy, FAI syndrome, and proximal hamstring tendinopathy. Hip dysfunction drives problems above and below — including the lower back and knee.
Learn more
Foot & Ankle
Plantar fasciopathy, Achilles tendinopathy, chronic ankle instability, and tibialis posterior tendinopathy. The foot is the fascial floor of the body — what happens here travels upward.
Learn more
Conveniently located in
the heart of Chelsea Heights.
Two minutes from the Mornington Peninsula Freeway. Serving Chelsea Heights, Mordialloc, Bonbeach, Edithvale, Aspendale, Patterson Lakes, Braeside, Waterways and Keysborough.
Suite 30, Level 1 / 93 Wells Rd, Chelsea Heights VIC 3196Entry via Benchmark Corporate Centre — between Advantage Pharmacy and Wells Road Medical Centre.
Mon & Wed 9am – 8pm · Tue & Thu 9am – 3:00pm3rd Saturday 9am – 1pm. Fri & Sun closed.
Ready to feel better?
Book your initial consultation online. Same-week appointments often available for new patients.
Book your appointment →
Or call us on (03) 9787 0600